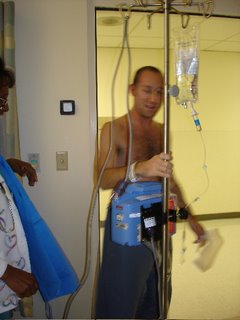
i just returned from the hospital, a day early! i thought a bit about what was going on, and realizing that there was no true reason for me to spend another night there, i made enough noise and kissed enough ass that they discharged me. there is something strangely addictive about being in the hospital that i am happy to have forced myself to escape. the bed is comfortable and adjustable, there is a table that blocks one side of the bed, the IV tree blocks the other side and is a pain to move around, nurses come to deliver anything at the touch of a button, and there is not really anywhere to go anyway, so it takes a lot of energy to motivate to get up out of the bed.
it is hard for me to describe how i am feeling. everything is so variable. i get tired all of a sudden, and then feel awake just as suddenly. i get waves of just feeling generally gross, but without any symptom specific enough to describe or treat. i have pangs of pain in strange locations, which come and go randomly. most constant, i think, is really just being in the mode of thinking of myself as a patient, and not as ME. it is very good that i was able to come back home even a little early, and regain some minimum semblance of normalcy.
the week at the hospital went better this time, everything was smoother and more organized, and i finally got set up with a competent hospital social worker, who not only comes up to my room, but whose services are included in the price of admission. side effects so far seem more mild than the first time around, but then again, it did take a few days for the cisplatin to wreak havoc, so i can't claim victory yet. they've switched me to what my night nurse linda calls the "beverly hills" anti-nausea medications, because the standard compazine+reglan had been so miserable. i can't wait to see the bill.
speaking of bills, one of the shocking things about this ordeal is the total disconnect between the delivery of services and the costs that they incur. none of the doctors or nurses have any idea nor do they care about what anything costs their patients. granted, most of us at this hospital have "good" insurance, but my "good" insurance only covers at 90%, and i can only make the roughest of estimates of how high the total will run in my case. $3-4000 a night, something like 25 nights, that's around $100k, not including any of the scans, all the medication, and office visits, which can't be cheap. i am conservatively estimating cracking $300k by the end of this, which means that $30k of that is mine to pay. outrageous. i am amoung the wealthiest and best connected people in the country, and this is a real burden! what about everyone else?! i probably saved myself and the insurance company a good chunk of money by pushing for being discharged a day early. while i guess it is nice that i don't feel pressured by the hospital to get out as quickly as possible, this seems like the other extreme.
Thursday, November 30, 2006
round 2
monday i entered the hospital for round two of POMB-ACE chemotherapy. as a reminder, here's how it works, in more detail than some of you care about, and less detail than intrigues some others:
this round 2 of 8 cycles, each of which lasts 2 weeks. i have 3 rounds of "POMB", which consist of vincristine, methotrexate, bleomycin, cisplatin, and seemingly hundreds of liters of saline. each round of POMB starts on a monday, and i am in-patient at norris/usc cancer hospital until sometime during the day on friday. i then go home for the weekend, the week, and the following weekend, until beginning the third round of POMB on monday, december 11. on december 25, i get "ACE", which is actinomycin D, cyclophosphamide, and etoposide. this round is out-patient, though i come in every day for a 3-4h infusion (which is probably more like 8h in this hospital with all the setup). there may be some possibility of doing the ACE regimen at another hospital, which opens the intriguing idea of heading up north for a bit, but that hasn't yet been ironed out. if my tumor markers are still high (a bad thing), then i get another in-patient cycle of POMB starting january 8; if the markers are normal, i stay for the same amount of time, but they don't give me the cisplatin (the big nasty P for platinum), which makes it "OMB". on january 22, i will get the out-patient ACE regimen, with a CT scan at the end. on february 5, i get OMB, and on february 19 i get ACE. we hope that there is no "after that...".
i have been feeling pretty good for the past few days before re-entering the hospital, and feel especially happy having spent them well, with friends and fun. my belly seems to have shrunken a little, maybe, and i am able to eat larger meals, and even get hungry at odd hours (i just ate four of grandma's brownies!). i am off the time-release morphine, which i just don't need right now, and as a result i am off all of the stool softeners and laxatives that went along with it, though my bowels are beginning their re-adjustment, which involves a definite and very uncomfortable overshoot. i even took a short nap this afternoon, which hasn't happened in a long while. i still seem to need sleeping pills for the night, though maybe tonight...? it is a relief to feel that despite the extremity of the situation, in general, it is going as well as it can.
i am back in the exact same room as last time, with many of the same nurses and doctors knocking on my door at all hours. the routine of the hospital is to be humored. i chit-chat with the night nurses who come in to change the saline, give me pills, and quiet my frequently demanding IV machine which beeps its displeasure. i guess at my weight before letting the nurse who keeps all of the vital statistics put me on the scale, and once she's taken my baseline blood oxygen measurements with that little glowy red thing on my finger, i hyperventilate to see if i can get the numbers to go up (it works, after about 20 seconds). i distract the over-worked second-year resident, sam, into spending half an hour with me at a time, talking about symptoms and coping mechanisms. the orderlies who bring in my food and take away cluttered trays have to negotiate a room teeming with procrastinating medical students who have come to visit. i have hung up a japanese scroll of swimming fish that florence brought for me, and my yellow submarine magnets will surely grace my metal door soon. walking around the ward and peeking into people's rooms, it is clear that i am somewhat of a novelty as far as patients go. i don't think that treat too many young, wisecracking medical students, with french girlfriends, mothers who stay the night, requesting rooms with wireless internet so he can run his blog (no luck: the two rooms that have it by chance are already occupied; i have to mosey down to the quad to post things, which is why it can take some time to post when i am in here). i do what i can to stay amused, and part of that is amusing others.
i feel conflicted about what to do with time like this when i am feeling good. on the one hand, the proportion of time that i spend feeling bad is so large that i think that i should take advantage of my "up" time to just relax and recuperate and enjoy life. on the other hand, the administration here at the medical school has done a good job at reinforcing the idea of professionalism, that being in medical school is less about learning a bunch of facts and being able to take multiple choice tests than about learning to be effective and engaged in the health care system. with this in mind, i feel an obligation to get something out of this experience other than merely making it through to the other side. it's not fair that this is happening to me, i don't deserve it, there is no master plan that put me on this path, but nonetheless i feel like i should make the most of these circumstances, and do what i can to see it as "opportunity" every now and then. there are so many issues that are brought up by this experience: so many glaring shortcomings in the system that deserve identification and possible future investment of my time, so many drugs that i am taking which i don't know enough about, so many alternative therapies to be investigated, in short, so many "productive" things that i could be doing with this time. i even thought about interviewing applicants to medical school from my bed - what better situation in which to evaluate someone's fitness for medicine? (what an intimidating interview! they certainly wouldn't forget the experience, that's for sure!).
this round 2 of 8 cycles, each of which lasts 2 weeks. i have 3 rounds of "POMB", which consist of vincristine, methotrexate, bleomycin, cisplatin, and seemingly hundreds of liters of saline. each round of POMB starts on a monday, and i am in-patient at norris/usc cancer hospital until sometime during the day on friday. i then go home for the weekend, the week, and the following weekend, until beginning the third round of POMB on monday, december 11. on december 25, i get "ACE", which is actinomycin D, cyclophosphamide, and etoposide. this round is out-patient, though i come in every day for a 3-4h infusion (which is probably more like 8h in this hospital with all the setup). there may be some possibility of doing the ACE regimen at another hospital, which opens the intriguing idea of heading up north for a bit, but that hasn't yet been ironed out. if my tumor markers are still high (a bad thing), then i get another in-patient cycle of POMB starting january 8; if the markers are normal, i stay for the same amount of time, but they don't give me the cisplatin (the big nasty P for platinum), which makes it "OMB". on january 22, i will get the out-patient ACE regimen, with a CT scan at the end. on february 5, i get OMB, and on february 19 i get ACE. we hope that there is no "after that...".
i have been feeling pretty good for the past few days before re-entering the hospital, and feel especially happy having spent them well, with friends and fun. my belly seems to have shrunken a little, maybe, and i am able to eat larger meals, and even get hungry at odd hours (i just ate four of grandma's brownies!). i am off the time-release morphine, which i just don't need right now, and as a result i am off all of the stool softeners and laxatives that went along with it, though my bowels are beginning their re-adjustment, which involves a definite and very uncomfortable overshoot. i even took a short nap this afternoon, which hasn't happened in a long while. i still seem to need sleeping pills for the night, though maybe tonight...? it is a relief to feel that despite the extremity of the situation, in general, it is going as well as it can.
i am back in the exact same room as last time, with many of the same nurses and doctors knocking on my door at all hours. the routine of the hospital is to be humored. i chit-chat with the night nurses who come in to change the saline, give me pills, and quiet my frequently demanding IV machine which beeps its displeasure. i guess at my weight before letting the nurse who keeps all of the vital statistics put me on the scale, and once she's taken my baseline blood oxygen measurements with that little glowy red thing on my finger, i hyperventilate to see if i can get the numbers to go up (it works, after about 20 seconds). i distract the over-worked second-year resident, sam, into spending half an hour with me at a time, talking about symptoms and coping mechanisms. the orderlies who bring in my food and take away cluttered trays have to negotiate a room teeming with procrastinating medical students who have come to visit. i have hung up a japanese scroll of swimming fish that florence brought for me, and my yellow submarine magnets will surely grace my metal door soon. walking around the ward and peeking into people's rooms, it is clear that i am somewhat of a novelty as far as patients go. i don't think that treat too many young, wisecracking medical students, with french girlfriends, mothers who stay the night, requesting rooms with wireless internet so he can run his blog (no luck: the two rooms that have it by chance are already occupied; i have to mosey down to the quad to post things, which is why it can take some time to post when i am in here). i do what i can to stay amused, and part of that is amusing others.
i feel conflicted about what to do with time like this when i am feeling good. on the one hand, the proportion of time that i spend feeling bad is so large that i think that i should take advantage of my "up" time to just relax and recuperate and enjoy life. on the other hand, the administration here at the medical school has done a good job at reinforcing the idea of professionalism, that being in medical school is less about learning a bunch of facts and being able to take multiple choice tests than about learning to be effective and engaged in the health care system. with this in mind, i feel an obligation to get something out of this experience other than merely making it through to the other side. it's not fair that this is happening to me, i don't deserve it, there is no master plan that put me on this path, but nonetheless i feel like i should make the most of these circumstances, and do what i can to see it as "opportunity" every now and then. there are so many issues that are brought up by this experience: so many glaring shortcomings in the system that deserve identification and possible future investment of my time, so many drugs that i am taking which i don't know enough about, so many alternative therapies to be investigated, in short, so many "productive" things that i could be doing with this time. i even thought about interviewing applicants to medical school from my bed - what better situation in which to evaluate someone's fitness for medicine? (what an intimidating interview! they certainly wouldn't forget the experience, that's for sure!).
Friday, November 24, 2006
celebrity
i have been profoundly moved by the generosity of spirit i have witnessed on the part of so many people. the outpouring of love has been stunning, and truly beautiful. i feel like i am surrounded by an immense cushion of affection, and you have all helped soften the blow considerably.
i had an awkward thought, though. it can't last. it's just a fact that you all are living full and busy lives, and that mine will remain dreary for a long time. the shock of bad news draws people together in spectacular ways, but the shock is transient. i would be willing to bet that my "celebrity" status has reached its apogee, and that the circle of people who remain engaged will quickly tail off. i am writing this for a number of reasons, and one of them is to tell YOU that i understand, and that you don't have to feel guilty about it. another reason to write it down is to prepare myself, to realize that it is natural, and not personal.
please don't get me wrong. i am BY NO MEANS saying that i want fewer visitors, loving comments left on this blog, warm emails, or loving calls. your support is absolutely wonderful, and brightens my days. i am merely trying to prepare myself for the long haul. this thing is going to last a minimum of four months, plus whatever else may need to happen medically, plus the time it takes to put my life back together (whatever that means). i don't know if this is a good idea psychologically, but it seems to me that i will eventually need to stop thinking of myself as in a crisis, and "normalize" this phase of my life to whatever degree possible.
not that i know what i am talking about. i have only just finished the first of eight two-week cycles, and while i am not feeling perfect, i have just had a couple of relatively comfortable and normal days, so it is easy for me to sound strong. i know that as the chemo really takes effect, and as my immune system gets pummeled, that i am in for a lot more unpleasantness. i can't imagine that the nastiness of the side effects will abate, and they will more than likely worsen.
so maybe what i am saying is that i hope that you will pace yourselves. i will need your love and support for a long time to come, under less shocking but possibly more difficult circumstances.
again, thank you all, from the bottom of my heart. i love you right back.
i had an awkward thought, though. it can't last. it's just a fact that you all are living full and busy lives, and that mine will remain dreary for a long time. the shock of bad news draws people together in spectacular ways, but the shock is transient. i would be willing to bet that my "celebrity" status has reached its apogee, and that the circle of people who remain engaged will quickly tail off. i am writing this for a number of reasons, and one of them is to tell YOU that i understand, and that you don't have to feel guilty about it. another reason to write it down is to prepare myself, to realize that it is natural, and not personal.
please don't get me wrong. i am BY NO MEANS saying that i want fewer visitors, loving comments left on this blog, warm emails, or loving calls. your support is absolutely wonderful, and brightens my days. i am merely trying to prepare myself for the long haul. this thing is going to last a minimum of four months, plus whatever else may need to happen medically, plus the time it takes to put my life back together (whatever that means). i don't know if this is a good idea psychologically, but it seems to me that i will eventually need to stop thinking of myself as in a crisis, and "normalize" this phase of my life to whatever degree possible.
not that i know what i am talking about. i have only just finished the first of eight two-week cycles, and while i am not feeling perfect, i have just had a couple of relatively comfortable and normal days, so it is easy for me to sound strong. i know that as the chemo really takes effect, and as my immune system gets pummeled, that i am in for a lot more unpleasantness. i can't imagine that the nastiness of the side effects will abate, and they will more than likely worsen.
so maybe what i am saying is that i hope that you will pace yourselves. i will need your love and support for a long time to come, under less shocking but possibly more difficult circumstances.
again, thank you all, from the bottom of my heart. i love you right back.
Thursday, November 23, 2006
getting old
i get told a lot that this experience will one day make me a better doctor, and i am even starting to believe it.
all of a sudden i feel a lot of sympathy for old people. for the first time in my life, i feel like i really can understand. the similarities are stunning: constant dependence on others; discomfort that will not go away; feeling like there are things that i used to do that are no longer possible, that who i was no longer exists; distrust of my own body; complaining all the time; boredom; uselessness; feeling like the world is going on without me; constant use of drugs that have unpleasant side effects; doctors who might be trying to help, but really can't make you feel all the way better; insomnia; hearing problems; isolation; emptiness; loss of identity, and gaining a new identity: that of "being sick".
all of a sudden i feel a lot of sympathy for old people. for the first time in my life, i feel like i really can understand. the similarities are stunning: constant dependence on others; discomfort that will not go away; feeling like there are things that i used to do that are no longer possible, that who i was no longer exists; distrust of my own body; complaining all the time; boredom; uselessness; feeling like the world is going on without me; constant use of drugs that have unpleasant side effects; doctors who might be trying to help, but really can't make you feel all the way better; insomnia; hearing problems; isolation; emptiness; loss of identity, and gaining a new identity: that of "being sick".
Wednesday, November 22, 2006
a fabulous night
every positive event seems like an accomplishment, something to take note of and value and cherish.
after a day of compazine/reglan induced hyperkinesia, tinnitus, and general craziness, i had a fabulous night filled with friends and love. jake, florence, paula, jehangeer, neil and jessica, caleb and coco came over, and flooded me with distraction, which is the only solace. i am happy to be active when i can, not only to move but to DO. we all walked to fatburger where i had three fries and a sip of lemonade-iced tea. tonight was the first night that i have tried getting high, and it was really a great decision. i was scared that it would put me in a bad head-space, but it allowed me to relax, to talk with people, to laugh my ass off, to introspect.
this is what i imagine it is like being pregnant: one is miserable, for a defined period of time that is not alterable, and yet the end result is something deeply desired (in this case, being done with it all and getting back to reality).
maybe the best description i have come up with so far is this: imagine that you are SUPER constipated, and you just KNOW that once you let things go, the whole outlook on everything will change, but until then, every moment of waiting, there is a gigantic distraction to rationality that is omnipresent. but this plug-up is going to last a while. the discomfort is so big that at every moment i need to find a way to occupy myself with some task. i must develop many different ways of coping. meditation. painting. guitar. yoga. dancing.
after a day of compazine/reglan induced hyperkinesia, tinnitus, and general craziness, i had a fabulous night filled with friends and love. jake, florence, paula, jehangeer, neil and jessica, caleb and coco came over, and flooded me with distraction, which is the only solace. i am happy to be active when i can, not only to move but to DO. we all walked to fatburger where i had three fries and a sip of lemonade-iced tea. tonight was the first night that i have tried getting high, and it was really a great decision. i was scared that it would put me in a bad head-space, but it allowed me to relax, to talk with people, to laugh my ass off, to introspect.
this is what i imagine it is like being pregnant: one is miserable, for a defined period of time that is not alterable, and yet the end result is something deeply desired (in this case, being done with it all and getting back to reality).
maybe the best description i have come up with so far is this: imagine that you are SUPER constipated, and you just KNOW that once you let things go, the whole outlook on everything will change, but until then, every moment of waiting, there is a gigantic distraction to rationality that is omnipresent. but this plug-up is going to last a while. the discomfort is so big that at every moment i need to find a way to occupy myself with some task. i must develop many different ways of coping. meditation. painting. guitar. yoga. dancing.
Tuesday, November 21, 2006
insanity
i just cant get over how much of a rigamarole it is to find a psychiatrist who is also able to speak emotionalese. granted, its thanksgiving and all, but craziness respects no calendar (remind me of that when i am on a psych rotation sometime). if anyone knows any psychiatrist+psychologists who take blue cross and are near the hollywood area, i need to talk with them! how can it be that they are so hard to find?
i awoke today with the strangest jittery clenchy jumpy cannot stop moving must keep moving keep moving every second must! it was terrible. a psychologist recommended by a friend dropped by at 10, and we talked for an hour as i jumped off of the walls. after many phone calls, it looks like it is the compazine+reglan that are giving me these "extra-pyramidal" symptoms, and I have stopped taking them altogether. now i am hoping that i just have to wait for my liver to catch up with this decision and get them out of my system. benadryl was recommended, and though this makes no sense, it helped a bit. i would rather be glurky than have parkinsons-like symptoms.
forcing myself to be social is a must.
i awoke today with the strangest jittery clenchy jumpy cannot stop moving must keep moving keep moving every second must! it was terrible. a psychologist recommended by a friend dropped by at 10, and we talked for an hour as i jumped off of the walls. after many phone calls, it looks like it is the compazine+reglan that are giving me these "extra-pyramidal" symptoms, and I have stopped taking them altogether. now i am hoping that i just have to wait for my liver to catch up with this decision and get them out of my system. benadryl was recommended, and though this makes no sense, it helped a bit. i would rather be glurky than have parkinsons-like symptoms.
forcing myself to be social is a must.
Monday, November 20, 2006
slow return
while i atill am not really sleeping, despite a serious intensification of my sleepytime meds, i have to say that things are looking up - i had a "normal" morning, if you can call it that, since i haven't had a normal morning since the last time i was jet lagged, but at least feeling reasonable, not overly keyed-up for no good reason, nor like my belly was going to explode at any minute. i am just going to have to get used to napping in twnety minute spurts whenever my body decides its time, and to ignore the hot flashes and agitation that comes with a totally mixed up endocrine system. it was nice to be able to just smile, and be easy, and relax, if only for an hour. my guts have decided that it is time to kick up some more dust, and thus i am writing, a way to distract and dissipate some of the errant energy fluttering around.
i am jumping through hoops in order to find some psychological services, which is really ridiculous in a situation like this. doesn't it seem like this kind of thing would just appear on my doorstep, all taken care of? if there's one thing sick people shouldn't have to deal with, it is making sure that they dont drive themselves crazy.
i am jumping through hoops in order to find some psychological services, which is really ridiculous in a situation like this. doesn't it seem like this kind of thing would just appear on my doorstep, all taken care of? if there's one thing sick people shouldn't have to deal with, it is making sure that they dont drive themselves crazy.
Sunday, November 19, 2006
sleep
the day passed so slowly, tucked between my groin and my liver. any change in orientation threatens upheaval, and every position attained is as unsatisfying as the last.
i felt two seconds of tingling in my right fingertips, just enough to scare me. peripheral neuropathy on its way? i may need to get back to painting and drawing my ultra-precision psychedelia while i still can.
we decided that today was going to have to be a day between just the two of us, which really was mostly to give amelie a break, because i am so incommunicado that she ends up having to do the entertaining if there is anyone else around. while it was nice to be alone, finally, the two of us, lack of sleep plus lack of comfort made for a vague and frustrating day for me, one that i will be happy to avoid repeating. activity is necessary for sanity. reading. writing. cooking, guitar. painting. whatever. life must have goals besides surviving, even if they are short term and inconsequential.
we slurped down some chinese medicinal soup made by a friend's mother, which was exactly what i needed to be eating. what is it, anyway, about chicken soup? bring on the voodoo, man, i'll take all i can get.
at around 9pm i couldnt handle it anymore, and took an ambien to check out for the evening. i've been in a semi-dream state ever since, which is lovely since for some reason i am not in pain or discomfort for the first time in ??! either my body is getting it's shit back together, or this is the perfect drug cocktail.
i felt two seconds of tingling in my right fingertips, just enough to scare me. peripheral neuropathy on its way? i may need to get back to painting and drawing my ultra-precision psychedelia while i still can.
we decided that today was going to have to be a day between just the two of us, which really was mostly to give amelie a break, because i am so incommunicado that she ends up having to do the entertaining if there is anyone else around. while it was nice to be alone, finally, the two of us, lack of sleep plus lack of comfort made for a vague and frustrating day for me, one that i will be happy to avoid repeating. activity is necessary for sanity. reading. writing. cooking, guitar. painting. whatever. life must have goals besides surviving, even if they are short term and inconsequential.
we slurped down some chinese medicinal soup made by a friend's mother, which was exactly what i needed to be eating. what is it, anyway, about chicken soup? bring on the voodoo, man, i'll take all i can get.
at around 9pm i couldnt handle it anymore, and took an ambien to check out for the evening. i've been in a semi-dream state ever since, which is lovely since for some reason i am not in pain or discomfort for the first time in ??! either my body is getting it's shit back together, or this is the perfect drug cocktail.
Saturday, November 18, 2006
vibrations
The world vibrates, it is divided into what is inside and what is outside by bowels. Sometimes my head is included in one category, sometimes the other.
While last night was not too uncomfortable, I didn’t sleep either, until about 6 when I let myself be convinced that putting ambien into my system wasn’t the straw that would break my liver’s back. The meds seem to be effective, at least as far as preventing outright nausea and pain, and the flow has remained largely mouth-to-anus, which is what really counts.
Everyone around me has invested so much of themselves into making this work, I am in awe, and humbled, and loved, and sad that it has come to this. How much of my own discomfort can I ignore, to bring less to others? How much of it am I making up to begin with? This sum seems large when I am feeling good, and then evaporates with the next pang and swim of the labyrinths. I couldn’t feed myself, was at the point of vomiting at the table, but five minutes later, Amelie could feed me as I was lying down, and it tasted wonderful.
Writing seems necessary, even as the inanity of the words accumulate on the screen. My head is so fuzzy that it will be a miracle if anything of interest materializes out of these meanderings. The idea was to have a blog, but who wants to read this, simple recounting of events and blurry scenes that go nowhere? I am used to holding myself to a higher standard. In a situation like this, though, the DOING is maybe more important than the result. So those of you who area reading this, keep that in mind. I don’t really know who this is for.
While last night was not too uncomfortable, I didn’t sleep either, until about 6 when I let myself be convinced that putting ambien into my system wasn’t the straw that would break my liver’s back. The meds seem to be effective, at least as far as preventing outright nausea and pain, and the flow has remained largely mouth-to-anus, which is what really counts.
Everyone around me has invested so much of themselves into making this work, I am in awe, and humbled, and loved, and sad that it has come to this. How much of my own discomfort can I ignore, to bring less to others? How much of it am I making up to begin with? This sum seems large when I am feeling good, and then evaporates with the next pang and swim of the labyrinths. I couldn’t feed myself, was at the point of vomiting at the table, but five minutes later, Amelie could feed me as I was lying down, and it tasted wonderful.
Writing seems necessary, even as the inanity of the words accumulate on the screen. My head is so fuzzy that it will be a miracle if anything of interest materializes out of these meanderings. The idea was to have a blog, but who wants to read this, simple recounting of events and blurry scenes that go nowhere? I am used to holding myself to a higher standard. In a situation like this, though, the DOING is maybe more important than the result. So those of you who area reading this, keep that in mind. I don’t really know who this is for.
the first week
Day 1 – Monday, November 13, 2006
With Amelie and my parents, I arrived at Norris Comprehensive Care Cancer Center at 7:30am. Dr Quinn, my oncologist, had put me at the head of the line, and while I felt bad knowing that there were more than a dozen people who would be sitting in the waiting room even longer throughout the day because of my priviledged acces, my guilt only penetrates so far.
The choices were bleak, and there was insufficient data to make a rational decision. I have non-seminomatous germ cell cancer that has spread to “non-pulmonary visceral sites”, which places me in a not-too-euphamistically named “poor” prognosis category. The outcome for this group is maybe not much better than flipping a coin when treated with the standard of care, BEP (bleomycin, etoposide, cisplatin (the “P” standing for the platinum in the latter)). Because these clearly aren’t acceptable numbers, there are lots of people around the world trying to find a more effective treatment. Thus far, these efforts have not been coordinated and systematized, and there have been few head-to-head randomized controlled trials comparing different regimens. Here at Norris, Dr Quinn has experience with POMB-ACE, which is a very intense regimen consisting of all of the ingredients of BEP, but in greater doses, plus some other chemotherapy drugs, for 16 weeks instead of 12. The toxicity is higher, with the scariest prospect being an increased risk (from 5% with BEP to 10% with POMB-ACE) of developing peripheral neuropathy. POMB-ACE has been shown elsewhere to be “non-inferior” to BEP treatment in terms of curing the cancer, but there is no published data to support an assertion that it is superior. In Dr Quinn’s experience, however, with between 30-40 patients on POMB-ACE, he has seen a 5-year survival rate of 70%, as opposed to only 40% with BEP.
It was yet another surreal situation. My parents, Amelie, and I were being asked to weigh the evidence, connect with our collective gut feelings, and make a decision post haste, because I would be starting immediately. We circled the couches in the waiting room to confer, which apparently pissed off the powers that be because we were offered an empty office in which to continue the drama. Pulling on all the strings we had, we conferred with the stars at UCSF and at Stanford, who did some calling of their own, and who came down more or less leaning toward POMB-ACE, despite it not being the standard of care at their own institutions. In the end, it was an analogy of my father’s that helped to pull together my own frayed ends of logic. We gotta hit this thing hard, hit it out of the goddamn park. I’m young, otherwise healthy, surrounded by support, and at a world-class institution. The risks of toxicity are there, and scary, but the possible jump in prognosis with the more intense regimen is just too big to ignore. Horribly enough, survival, not side effects, have to be the primary focus around here.
While this is not a high “level of evidence” to be acting upon, I feel confident about it being a good decision. Of course, nobody will ever know.
We told Quinn of our decision, and then proceeded to admitting, where we waited, and waited, and waited for a room, for hours upon hours, with knotted stomachs, snotty faces, and uncontrollable sighing. I didn’t get put in my room until around 4pm, the IV didn’t get started until 7, and then I had to wait around, peeing out saline and trying not to lose my mind before the chemo finally arrived at 11:30pm. It was a moment I will never forget, as I looked into my mother’s eyes, and she sang Joe Cocker’s “You are so beautiful”, as the first of the life giving poison slipped into my veins.
Day 2 - Tuesday
Not a moment free! There was a parade of medical students, five at a time, from the moment that they got out of their review session at noon until 6pm. I’ve got to set up a blog and get people to read it before they come in, so I don’t have to repeat myself ad nauseum. But it is great to be surrounded by so much love and support. Taking a stroll with My Buddy the IV machine out to the quad is to invite neck rubs and a crowd of people forming around. Having chosen this relatively unique treatment regimen means that it will be much less easy to move my treatment up north if I feel like I need to, and this was one of the factors that made me hesitant about it. But now that I am here for the duration, I can reflect on the positives of the situation, and it is wonderful to have hundreds of people around, all the time, to keep me distracted and amused
Day 3 - Wednesday
After a long night of hiccups with thorazine and baclofan to try to stave them off (with unimpressive results), being awoken and reawoken for fluid intake/output and various drugs, and having to reset my IV pump every time I did fall asleep and bent my arm in the wrong way, it was a groggy morning.
It was time to put in the PICC line. In my second-year med student mind, there is only one association that I have mamaged to make with PICC lines, which is that they equal hospital-acquired infections. I required a fair bit of convincing before agreeing to it. Before I went down to the PICC nurse, I was hiccupping, and they decided to give me a “double dose” (whatever that means) of IV thorazine, on top of whatever thorazine and baclofam I had already consumed in pill form. It was a pretty miserable experience, though I am not sure why. I was just so loopy and floppy and sleepy that I couldn’t keep my shit together, but I also couldn’t sleep. I remember the PICC nurse saying that they should shoot everyone up with thorazine before sending them to her, because she had never had such a compliant patient. My delirium lasted a good four hours, but it was not a fun kind of stoned. The PICC line is great, though – I have full mobility of my arm because it’s inserted above my elbow instead of right in it, it doesn’t ache like the normal lines, and my IV machine doesn’t need to be babied in order to function.
The time that I spend in front of this keyboard is pretty much all of the “free” time that I have had. There is so much media in this room that I am definitely not going to get to until I return home – books, music, recorded books, movies.
Thursday
I weigh 179lbs! That’s 30 more than usual. My belly is inflated beyond belief, with the 15lbs of tumor matched by three and a half days of poop and liters of saline that hasn’t found its way out yet. They are pumping me up fast with saline, because we’re dropping the bomb on the nasties in an hour: cisplatin’s gonna ‘splat-em. And me, apparently. So far, I’ve completely escaped from nausea, but I don’t know how much longer that is going to last.
The day went OK, with the only real problem being from the laxatives which made me crampy and gassy. The chemo was like being on lots of coffee and wanting to sleep and walk and fart and lie down and talk and do tai chi and eat and sit all at once.
It was almost as emotional to finish the first round of chemo as it had been to start it. While this one will go better and easier than all the rest, at least I know a little of what to expect. I do have to say that there are lots of dropped balls around here, always with plausible explanations (one of the nurses didn’t show up for work, the IV didn’t get changed because the timing worked out right at the changing of the shift, etc), but nonetheless inconsistent results. There have been too many times when I have had to cajole for more pain meds.
Friday
An MRI had been ordered to check for the possibility of brain metastases, and since Norris doesn’t have an MRI machine, it had to happen 200 yards away at University Hospital, which apparently required the use of an ambulance and two EMTs. Just how inefficient can we make this system? I honestly could have walked. The whole MRI experience was super trippy, with loud techno sci-fi sound effects mingling with Sting piped in over headphones, and don’t move! as the machine clunks and bumps its way to ultra-precision imaging. Makes no sense. But the results are back and clear, well, kind of – there was an incidental finding of an AVM, which is just not something that I want to think about right now. Ugh. Another long day of waiting, this time to be discharged. Norris is not a very organized place.
Being at home, without electronic beeping pumping dog of an IV machine following me around everywhere, is fantastic. Sleep when I want to, if I can, and at least have the option of eating great food, even if I can’t necessarily get it down.
This feeling is most like coming down after acid, cracked out day 2 without having had a fun day 1 to vibrate. Just the willies, the non-specifics. Am I asleep or not? Apparently not, since I am typing. But not for long.
With Amelie and my parents, I arrived at Norris Comprehensive Care Cancer Center at 7:30am. Dr Quinn, my oncologist, had put me at the head of the line, and while I felt bad knowing that there were more than a dozen people who would be sitting in the waiting room even longer throughout the day because of my priviledged acces, my guilt only penetrates so far.
The choices were bleak, and there was insufficient data to make a rational decision. I have non-seminomatous germ cell cancer that has spread to “non-pulmonary visceral sites”, which places me in a not-too-euphamistically named “poor” prognosis category. The outcome for this group is maybe not much better than flipping a coin when treated with the standard of care, BEP (bleomycin, etoposide, cisplatin (the “P” standing for the platinum in the latter)). Because these clearly aren’t acceptable numbers, there are lots of people around the world trying to find a more effective treatment. Thus far, these efforts have not been coordinated and systematized, and there have been few head-to-head randomized controlled trials comparing different regimens. Here at Norris, Dr Quinn has experience with POMB-ACE, which is a very intense regimen consisting of all of the ingredients of BEP, but in greater doses, plus some other chemotherapy drugs, for 16 weeks instead of 12. The toxicity is higher, with the scariest prospect being an increased risk (from 5% with BEP to 10% with POMB-ACE) of developing peripheral neuropathy. POMB-ACE has been shown elsewhere to be “non-inferior” to BEP treatment in terms of curing the cancer, but there is no published data to support an assertion that it is superior. In Dr Quinn’s experience, however, with between 30-40 patients on POMB-ACE, he has seen a 5-year survival rate of 70%, as opposed to only 40% with BEP.
It was yet another surreal situation. My parents, Amelie, and I were being asked to weigh the evidence, connect with our collective gut feelings, and make a decision post haste, because I would be starting immediately. We circled the couches in the waiting room to confer, which apparently pissed off the powers that be because we were offered an empty office in which to continue the drama. Pulling on all the strings we had, we conferred with the stars at UCSF and at Stanford, who did some calling of their own, and who came down more or less leaning toward POMB-ACE, despite it not being the standard of care at their own institutions. In the end, it was an analogy of my father’s that helped to pull together my own frayed ends of logic. We gotta hit this thing hard, hit it out of the goddamn park. I’m young, otherwise healthy, surrounded by support, and at a world-class institution. The risks of toxicity are there, and scary, but the possible jump in prognosis with the more intense regimen is just too big to ignore. Horribly enough, survival, not side effects, have to be the primary focus around here.
While this is not a high “level of evidence” to be acting upon, I feel confident about it being a good decision. Of course, nobody will ever know.
We told Quinn of our decision, and then proceeded to admitting, where we waited, and waited, and waited for a room, for hours upon hours, with knotted stomachs, snotty faces, and uncontrollable sighing. I didn’t get put in my room until around 4pm, the IV didn’t get started until 7, and then I had to wait around, peeing out saline and trying not to lose my mind before the chemo finally arrived at 11:30pm. It was a moment I will never forget, as I looked into my mother’s eyes, and she sang Joe Cocker’s “You are so beautiful”, as the first of the life giving poison slipped into my veins.
Day 2 - Tuesday
Not a moment free! There was a parade of medical students, five at a time, from the moment that they got out of their review session at noon until 6pm. I’ve got to set up a blog and get people to read it before they come in, so I don’t have to repeat myself ad nauseum. But it is great to be surrounded by so much love and support. Taking a stroll with My Buddy the IV machine out to the quad is to invite neck rubs and a crowd of people forming around. Having chosen this relatively unique treatment regimen means that it will be much less easy to move my treatment up north if I feel like I need to, and this was one of the factors that made me hesitant about it. But now that I am here for the duration, I can reflect on the positives of the situation, and it is wonderful to have hundreds of people around, all the time, to keep me distracted and amused
Day 3 - Wednesday
After a long night of hiccups with thorazine and baclofan to try to stave them off (with unimpressive results), being awoken and reawoken for fluid intake/output and various drugs, and having to reset my IV pump every time I did fall asleep and bent my arm in the wrong way, it was a groggy morning.
It was time to put in the PICC line. In my second-year med student mind, there is only one association that I have mamaged to make with PICC lines, which is that they equal hospital-acquired infections. I required a fair bit of convincing before agreeing to it. Before I went down to the PICC nurse, I was hiccupping, and they decided to give me a “double dose” (whatever that means) of IV thorazine, on top of whatever thorazine and baclofam I had already consumed in pill form. It was a pretty miserable experience, though I am not sure why. I was just so loopy and floppy and sleepy that I couldn’t keep my shit together, but I also couldn’t sleep. I remember the PICC nurse saying that they should shoot everyone up with thorazine before sending them to her, because she had never had such a compliant patient. My delirium lasted a good four hours, but it was not a fun kind of stoned. The PICC line is great, though – I have full mobility of my arm because it’s inserted above my elbow instead of right in it, it doesn’t ache like the normal lines, and my IV machine doesn’t need to be babied in order to function.
The time that I spend in front of this keyboard is pretty much all of the “free” time that I have had. There is so much media in this room that I am definitely not going to get to until I return home – books, music, recorded books, movies.
Thursday
I weigh 179lbs! That’s 30 more than usual. My belly is inflated beyond belief, with the 15lbs of tumor matched by three and a half days of poop and liters of saline that hasn’t found its way out yet. They are pumping me up fast with saline, because we’re dropping the bomb on the nasties in an hour: cisplatin’s gonna ‘splat-em. And me, apparently. So far, I’ve completely escaped from nausea, but I don’t know how much longer that is going to last.
The day went OK, with the only real problem being from the laxatives which made me crampy and gassy. The chemo was like being on lots of coffee and wanting to sleep and walk and fart and lie down and talk and do tai chi and eat and sit all at once.
It was almost as emotional to finish the first round of chemo as it had been to start it. While this one will go better and easier than all the rest, at least I know a little of what to expect. I do have to say that there are lots of dropped balls around here, always with plausible explanations (one of the nurses didn’t show up for work, the IV didn’t get changed because the timing worked out right at the changing of the shift, etc), but nonetheless inconsistent results. There have been too many times when I have had to cajole for more pain meds.
Friday
An MRI had been ordered to check for the possibility of brain metastases, and since Norris doesn’t have an MRI machine, it had to happen 200 yards away at University Hospital, which apparently required the use of an ambulance and two EMTs. Just how inefficient can we make this system? I honestly could have walked. The whole MRI experience was super trippy, with loud techno sci-fi sound effects mingling with Sting piped in over headphones, and don’t move! as the machine clunks and bumps its way to ultra-precision imaging. Makes no sense. But the results are back and clear, well, kind of – there was an incidental finding of an AVM, which is just not something that I want to think about right now. Ugh. Another long day of waiting, this time to be discharged. Norris is not a very organized place.
Being at home, without electronic beeping pumping dog of an IV machine following me around everywhere, is fantastic. Sleep when I want to, if I can, and at least have the option of eating great food, even if I can’t necessarily get it down.
This feeling is most like coming down after acid, cracked out day 2 without having had a fun day 1 to vibrate. Just the willies, the non-specifics. Am I asleep or not? Apparently not, since I am typing. But not for long.
intro
Last April, my loitering hand came across a bump in the night. Hard, painless, irregular, and projecting out from the otherwise smooth surface of my right testicle, as a first-semester second-year medical student, I “knew” what it was, or thought I did. The resident at Family Medicine the next day didn’t feel anything, and dismissed my concern as a symptom of the well-known hypochondriacal Medical Student’s Disease (MSD). I was unconvinced, and demanded to see the radiologist, who likewise regaled me of stories of his own MSD lymphoma as he smeared my nether regions with cold gel and started smooshing around with the ultrasound transducer. At a certain point, his story became fragmented, hesitant, and then stopped altogether, as a frown crept across his face. There was no easy way to tell me. I had been right. It was a solid tumor. He walked me back over to Family Medicine in order to make up for his faux pas and to ensure that I got taken seriously on the other end. As he spoke with the attending in the hallway, the original resident peeked her head into the room, beamed a great big smile, and trying not to laugh, asked “So? What did the radiologist tell you?” – “That it’s a tumor” – “(snicker) No, really. It’s nothing, right?”
She got straightened out. I received lots of apologetic voicemails from her over the next few weeks, which I never returned. I had more important things to take care of.
To make a very long story very short, everything pretty much went peachy. After surreal trips to the sperm bank in West LA, much organizing, agonizing, and weasling, I got the first surgery out of the way within a week. I went on to finish up the school year (with a lot of help from my friends), flew up to the Bay and had the second surgery, a retroperitoneal lymph node dissection, done at UCSF at the beginning of June. I was back in school, placing ever-more complicated pieces of a laser-cut jigsaw puzzle of life together, when a routine CT reminded me that it was not normal to have developed a beer belly within the span of a couple of weeks.
And blammo! Suddenly everything, everything, everything, is up in the air.
She got straightened out. I received lots of apologetic voicemails from her over the next few weeks, which I never returned. I had more important things to take care of.
To make a very long story very short, everything pretty much went peachy. After surreal trips to the sperm bank in West LA, much organizing, agonizing, and weasling, I got the first surgery out of the way within a week. I went on to finish up the school year (with a lot of help from my friends), flew up to the Bay and had the second surgery, a retroperitoneal lymph node dissection, done at UCSF at the beginning of June. I was back in school, placing ever-more complicated pieces of a laser-cut jigsaw puzzle of life together, when a routine CT reminded me that it was not normal to have developed a beer belly within the span of a couple of weeks.
And blammo! Suddenly everything, everything, everything, is up in the air.
Subscribe to:
Comments (Atom)